Help Us Fight Prostate Cancer
PSA Testing
The PSA test is a simple blood test that can help diagnose prostate problems, including prostate cancer.
The PSA test is a blood test that measures the amount of prostate specific antigen (PSA) in your blood. PSA is a protein produced by normal cells in the prostate and also by prostate cancer cells. It is measured in nanograms per millilitre in the blood and readings can register from less than 1 to over 1000. Readings of below 2 are considered normal in men below 50 rising to 5 in men aged 70+.
It’s normal to have a small amount of PSA in your blood, and the amount rises slightly as you get older and your prostate gets bigger. A raised PSA level (or if the PSA is rising more quickly than would be expected) may suggest you have a problem with your prostate, but not necessarily cancer.

What are my risks of getting prostate cancer?
There are some things that may mean men are more likely to get prostate cancer – these are called risk factors. There are three main risk factors :
Early Prostate cancer is often symptomless, meaning men are typically unaware they have prostate cancer until they get a PSA test. Be aware of the risks. If you have any of these risk factors, or have any symptoms, don’t wait, talk to your GP about getting a simple PSA blood test.
If caught early, it is usually curable. So GET TESTED!

Men have a right to be tested for prostate cancer on a regular basis via their GP if they are aged 50 or over. There is currently no national screening programme, but instead an informed choice programme, called prostate cancer risk management (click here to download PDF) for healthy men aged 50 or over who ask their GP about PSA testing. It aims to give men good information on the pros and cons of a prostate specific antigen (PSA) test.
The PSA test is not perfect: it will not help find all prostate cancers, it will miss some and will detect some that would never go on to cause harm. You can use use the Prostate Cancer UK online Risk Checker first and the UK Office for Health Improvement has also produced an information sheet : “PSA testing and prostate cancer: advice for men without symptoms of prostate disease” which should help you decide if you want to have the test or not. It is your decision. Before making your decision you may want to talk to your GP, practice nurse and your partner, family member or a friend.. If you decide to go ahead, your GP can arrange for it to be carried out free on the NHS.
However, we are aware that some doctors do not support prostate cancer testing with this test, especially if men present with no obvious symptoms. It might help to take a print out of this leaflet to give to your GP to explain why you are entitled to a test.
Should I get Tested?
The PSA test isn’t perfect, and it’s important to know the pros and cons. It’s up to you to decide whether having the test is the right thing for you. To help you decide if you would like a test the following video produced by the Surrey and Sussex Cancer Alliance and Medefer, of our Trustee, Prof Stephen Langley, may be helpful
Where do I get a PSA Test?
You can get a PSA Test at:
What happens if my PSA level is higher than it should be
Raised levels of PSA can indicate the presence of prostate cancer cells. However, this can also be due to a range of other factors, such as a urinary infection, an enlarged prostate, vigorous exercise or having had sex within the previous 48 hours.
The PSA blood test is the first step towards a diagnosis. It isn’t accurate enough to tell for certain if a man has prostate cancer or not. This means men need further tests, including a biopsy to confirm whether they have the disease. Men with raised PSA readings will only undergo a biopsy once they have also had an MRI scan (which generates detailed images of the prostate) to give vital clues as to whether it’s cancer, how big the cancer is and whether it appears to be at risk of spreading.
It is believed the current diagnostic pathway, including mpMRI, targeted biopsy and transperineal biopsy, has reduced the harms of over-diagnosis, with evidence showing that over-treatment rates have also reduced with active surveillance chosen more consistently by men with low and low/intermediate risk localised prostate cancer.
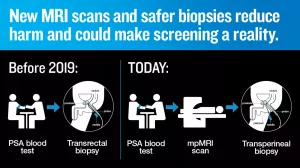
Image copyright Prostate Cancer UK
Two new techniques have been crucial to the new diagnostic pathway – multi parametric MRI scans (mpMRI) and transperineal guided biopsy (the needle is inserted into the perineum rather than the rectum, giving a lower risk of infection).
Before 2019, men with a high level of PSA in their blood were sent straight for a biopsy, which could cause pain and bleeding, and came with a risk of serious infection. These biopsies could also sometimes miss the cancer, leading to repeated biopsies with further risks of infection and uncomfortable side-effects.
Having a mpMRI scans beforehand could safely rule out many of these biopsies as unnecessary, as well as improving the accuracy of those that were needed, making them more likely to detect the cancer the first time.
PSA is not a perfect test but some large studies suggest it is about as effective as breast cancer screening in terms of picking up early cancers.
The European study of screening for prostate cancer, a long-running investigation into the value of PSA testing, found that it reduced deaths by up to 22 per cent over an 11-year period, according to results published in The Lancet in 2014.
Men will have a biopsy only if the MRI scan results warrant it, with the hope to distinguish not only that the raised PSA is due to cancer, but to separate the tigers (aggressive cancer) from the pussycats (slow growing) at an early stage and, in the process, reduce the rate of unnecessary biopsies by up to 30 per cent.
Get Tested!
Watch our animation explaining why it’s so important to catch Prostate Cancer early
